 Lateral decubitus positions6,13 or in patients obtunded Prolonged limb compression, as in Trendelenburg and.Cast or splint, especially if placed before removal of.Tight circumferential dressings (eg, can occur with.Strenuous exercise, especially in previously sedentaryĬonditions that Lead to a Reduction in Volume of.Decreased serum osmolarity (eg, nephritic syndrome11). 
Anabolic steroid use, resulting in muscle hypertrophy10.Reperfusion after prolonged periods of ischemia.Extravasations of arthroscopic fluid (eg, after routine.Infusions or high-pressure injections (eg, regional.Increased capillary permeability after burns (especially.High-energy trauma, as from high-speed motor vehicle.Revascularization of limb after ischemia.Hemorrhage: Vascular injury, coagulopathy.The adjacent compartments, may lead to compartment Open fractures, which should theoretically decompress.Soft tissue crush injuries without fractures in 23% of.Closed tibial shaft fractures (40%) and closed forearm.Direct soft tissue trauma with or without long boneįracture (10%–20% incidence after closed fracture).Conditions that Increase the Compartment Volume Diminished blood flow to local nerves first manifests as sensory changes. This, in turn, leads to a vicious cycle of continued fluid loss, further increasing tissue pressure and injury. Hypoxic injury causes cells to release free radicals, which increases endothelial permeability. The pressure at which this occurs is not known however, it is generally agreed that compartmental pressures greater than 30 mm Hg require emergent intervention because ischemia is imminent. However, as tissue pressure increases, extrinsic venous luminal pressure is exceeded, resulting in vein collapse. Under physiologic circumstances, the venous pressure exceeds that of the interstitial tissue pressure, sustaining venous outflow. If prolonged, permanent myoneural tissue damage occurs. As the compartmental pressure increases, the tissue hypoperfusion results in tissue hypoxia impeding cellular metabolism. Because various osseofascial compartments have a relatively fixed volume, introduction of excess fluid or external constriction increases pressure within the compartment and decreases tissue perfusion ( Figure 1). However, the entire mechanism of compartment syndrome is unclear. PathophysiologyĬompartment syndrome is essentially soft tissue ischemia, generally associated with trauma, fracture with subsequent casting, prolonged malpositioning during surgery, or reperfusion injury. Examples of factors leading to these changes are presented in Table 1. 
EtiologyĪny condition that can reduce the volume of the compartment or increase the size of the contents of the compartment can lead to an acute compartment syndrome. Only after about 40 years (since the 1970s) has the importance of measuring compartmental pressures become apparent. Jepson described ischemic contractures in dog hind legs, resulting from limb hypertension after experimentally induced venous obstruction. The consequences of persistently elevated intra-compartmental pressures were first described by Richard von Volkmann, who documented nerve injury and late muscle contracture from compartment syndrome after supracondylar fracture of the distal humerus.  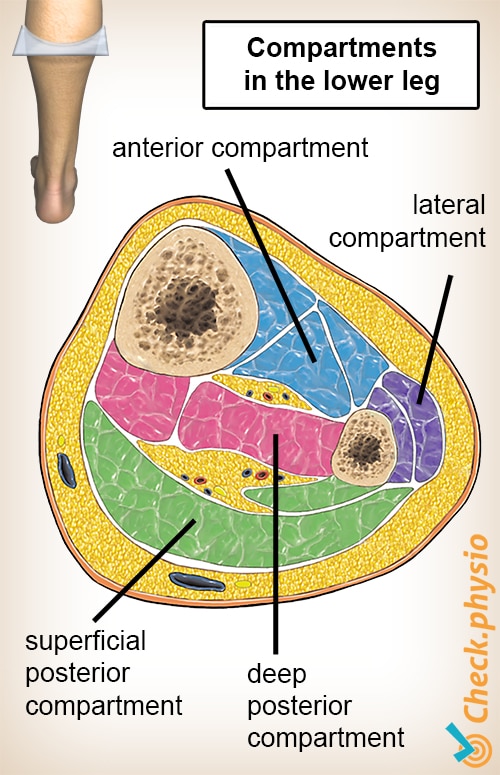
Acute compartment syndrome occurs more commonly in one of the four smaller compartments of the lower leg. In theory, the upper leg muscles are at a lower risk for injury than are the smaller muscles of the lower leg, because the muscles of the thigh can dissipate the large forces of direct trauma, causing less muscle injury and resultant edema. If missed, compartment syndrome can be a limb- and life-threatening condition.Ĭompartment syndrome is most common in the lower leg and forearm, although it can also occur in the hand, foot, thigh, and upper arm. These compartments enclose skeletal muscles along with the neurovascular structures that pass through the compartments. The musculoskeletal structures of the limbs are enclosed within compartments created by investing fascial layers with a limited ability to stretch. Regardless, practitioners should be aware of the patient risk factors, clinical presentation, and management of this potentially limb-threatening condition. Although regional anesthesia is often thought to delay diagnosis and treatment of acute compartment syndrome (ACS), there are only isolated case reports and a lack of evidence-based information to guide the clinical practice. It is an acute condition of the limbs in which the pressure of isolated or groups of poorly compliant muscle compartments increases dramatically and limits local soft tissue perfusion to the point of motor and sensory impairment and neuronal and tissue ischemic necrosis. Table of Contents Acute Compartment Syndrome of the Limb: Implications for Regional Anesthesia INTRODUCTIONĬompartment syndrome is an orthopedic emergency. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
